Abstract
Introduction: Venous thromboembolism (VTE) is common in patients with cancer. Non-O blood type is associated with higher levels of factor FVIII activity and von Willebrand factor compared to blood type O, and has been identified as a risk factor for VTE in the general population. However, the impact of ABO blood type on risk of cancer-associated VTE has not been clarified.
Methods: To determine the influence of non-O blood type on risk of cancer-associated VTE, we utilized the dataset of the Vienna Cancer and Thrombosis Study (CATS), which is a single center, prospective observational cohort study including patients with newly diagnosed or recurrent cancer. Patients were followed for objectively diagnosed, independently adjudicated VTE for a maximum of 2 years. VTE was quantified in competing risk analysis, accounting for all-cause mortality as competing outcome event. A proportional sub-hazard regression model according to Fine & Gray was used for between-group comparisons. Based on the violation of the proportional sub-hazard assumption, we explored potential time-dependent effects of non-O blood type on VTE risk in a restricted cubic spline analysis, modeling differences in risk estimates over follow-up time. Further, time-restricted subdistribution hazard ratios (SHR) were obtained specifically for the <3 months and ≥3 months follow-up intervals. In a subgroup analysis, differences in VTE risk according to ABO-blood type were analyzed for patients with very high thrombotic risk tumor types (pancreatic, gastric, glioblastoma), compared to the remainder of patients.
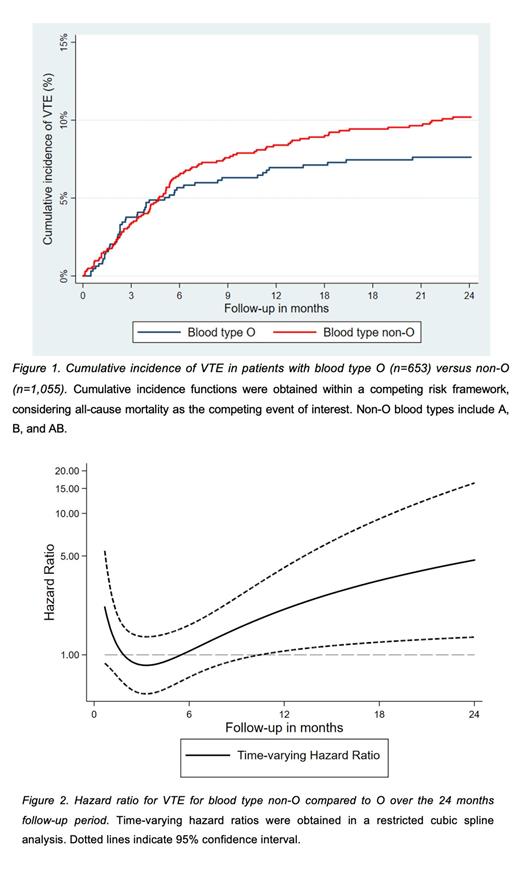
Results: In total, 1,708 patients were included in our analysis (46% female, median age: 61 years [interquartile range, IQR: 52-68]). The most common tumor types were lung (19%), breast (16%), and brain (14%) cancer, with 32% of solid tumor patients having metastatic disease at study inclusion. Over a median follow-up of 24 months (IQR: 10-24), 151 patients were diagnosed with VTE (cumulative 2-year incidence: 9.2%, 95% confidence interval [CI]: 7.9-10.7) and 649 patients died (2-year mortality: 38%). Overall, blood type O was present in 38% of patients, A in 40%, B in 15%, and AB in 7%. The cumulative incidence of VTE at 3-, 6-, 12-, and 24-months for patients with blood type O was 3.8% (95% CI: 2.5-5.5), 5.7% (95% CI: 4.1-7.7), 7.0% (95% CI: 5.1-9.1), and 7.6% (95% CI: 5.7-9.9), compared to 3.4% (95% CI: 2.4-4.7), 6.5% (95% CI: 5.1-8.1), 8.4% (95% CI:6.8-10.2), and 10.2% (95% CI: 8.4-12.2) in patients with non-O blood type (Gray´s test: p=0.103, Figure 1). Upon visual inspection of cumulative incidence functions, a violation of the proportional sub-hazard assumption was suspected. In restricted cubic spline analysis, estimating hazard ratio (HR) for VTE of patients with non-O compared to O blood type, a time-varying effect of non-O blood type towards an increased VTE risk was observed (Figure 2). Based on that, time-restricted competing risk regression models were performed. During the first 3 months of follow-up, no differences in VTE risk were found (SHR for non-O vs. O blood type: 1.00, 95% CI: 0.60-1.67, p=0.992). Beyond the first 3-month follow-up, patients with non-O blood type had an increased VTE risk compared to patients with blood type O (SHR 1.79, 95%CI: 1.12-2.85, p=0.015). In a subgroup analysis, no association with VTE risk was found in patients with very high thrombotic risk tumor types (SHR 0.94, 95% CI: 0.55-1.61, p=0.824). In contrast, in patients with low/intermediate risk cancer, non-O blood type was associated with increased risk of VTE (SHR 1.73, 95% CI: 1.09-2.73, p=0.019).
Conclusion: Non-O blood type was identified as a time dependent risk factor for cancer-associated VTE. In the first 3 months after study inclusion, characterized as the highest VTE risk period in our cancer cohort, no differences in VTE risk between blood types were found. Afterwards, beyond the first 3 months of follow-up, an increased VTE-risk in non-O blood types was observed, comparably in magnitude to the risk difference in the general non-cancer population. Further, an association of non-O blood type with VTE risk in patients with low/intermediate thrombotic risk cancers was observed, whereas no effect was present in those with very high-risk tumors. These findings indicate non-O blood type as a putative risk factor for VTE in patients with cancer in comparably low thrombotic risk scenarios.
Pabinger: Pfizer: Consultancy, Honoraria; Amgen: Consultancy, Honoraria; Novartis: Consultancy, Honoraria; Alexion: Consultancy, Honoraria; Daiichi Sanchyo: Consultancy, Honoraria; Takeda: Consultancy, Honoraria; Bayer: Consultancy, Honoraria; NovoNordisk: Consultancy, Research Funding; CSL Behring: Consultancy, Honoraria, Research Funding.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal